Pregnancy
Is Pregnancy Possible After Vasectomy?

Last Updated on March 28, 2026 by Joshua Isibor
Pregnancy after vasectomy is very possible, though the chances are smaller when compared to before vasectomy. So in this article, I’m going to explain possible ways to achieve pregnancy after vasectomy.
First, let’s get to understand more what vasectomy is!
WHAT IS VASECTOMY?
Vasectomy is a minor surgical procedure whereby the vas deferentia, which are ducts that carry sperm from the testicles to the seminal vesicles are cut, tied, sealed, seared, or otherwise interrupted. It is said to be a permanent birth control procedure. There is a scalpel approach, but recently a non- scalpel approach is applauded, though both give the same result.
In the non-scalpel approach, no incisions are made, locking forceps with a sharp tip, is used to puncture through the skin of the scrotal sac, or a special tear is made in the scrotal sac, with a special hemostat, the vas deferens is then grasped with a special clamp and tied off.
After a vasectomy, there is no effect on urination, ejaculation, erection, and libido. The male sexual life actually remains the same, there is still the production of sperm, but the body reabsorbs the sperm, and the male still produces semen, just that the semen do not contain sperm for the fertilization of the female egg, leading to no pregnancies.
RECANALIZATION
Also, there is a possibility that the Vas deferens can grow back together after vasectomy, and there is a possibility of pregnancy occurring, if the individual has intercourse. This occurs the first 6-8 weeks after vasectomy. Recanalization is likely to happen when ; one chooses an open-ended vasectomy which closes only one end of the vessel.
So it is advised to go for a lab test weeks after vasectomy, to ascertain that there are no sperm in the semen, and it should be certified by your doctor.
There are certain reasons that would make a couple consider pregnancy after vasectomy, such reasons include:
1) Death of a child
2) Death of a spouse
3) Divorce.
4) Change of condition that would have made them take a vasectomy decision.
So it’s advisable to consider these reasons before deciding on vasectomy as a birth control option.
Well! Let us call that a crash course on vasectomy, so let us get down to the business of the day; different approaches for possibilities of pregnancy after vasectomy.
In this article, I’m going to let you on two different approaches to pregnancy after vasectomy.
1.Vasectomy reversal.
2. Sperm retrieval.
VASECTOMY REVERSAL
This is also a minor surgical procedure in which the severed Vas deferens is reconnected and returned to their anatomical place. Vasectomy reversal is possible for about 20 years or longer, after vasectomy. But the longer the individual stays after vasectomy before a reversal, the less likely the possibility to achieve pregnancy.
This is the only procedure that leads to natural conception if successful.
There are two ways to carry out vasectomy reversal, but the quality of the sperm observed in the vassal fluid is important to decide which procedure to use ;
VASOVASOSTOMY –
Hmm, all these medical terms seem confusing and ambiguous right? Well, I will try to explain them in simple terms, okay.
During vasovasostomy the separated ends of each severed Vas deferens are reconnected medically, using stitches and sutures. If this procedure is successful this procedure will enable sperm to flow from the testicles again. There are 2 techniques to reconnect the Vas deferens during Vasovasostomy
Single-layer closure –
This involves stitching the outer layer of each severed end of the Vas deferens together, with a fine suture thread, this technique takes less time, but sometimes less successful.
Double layer closure –
This technique involves stitching the inner layer of each severed end of the tube first and then stitching the outer layer before reconnection is established and the scrotal incisions closed.
Vasovasostomy takes two to three hours to perform depending on the complexity of the surgery and the experience of the surgeon in charge. If a successful vasovasostomy is done, the average time for achieving pregnancy after the vasovasostomy is one year, though this is not certain, a good sperm count usually returns within three to six weeks.
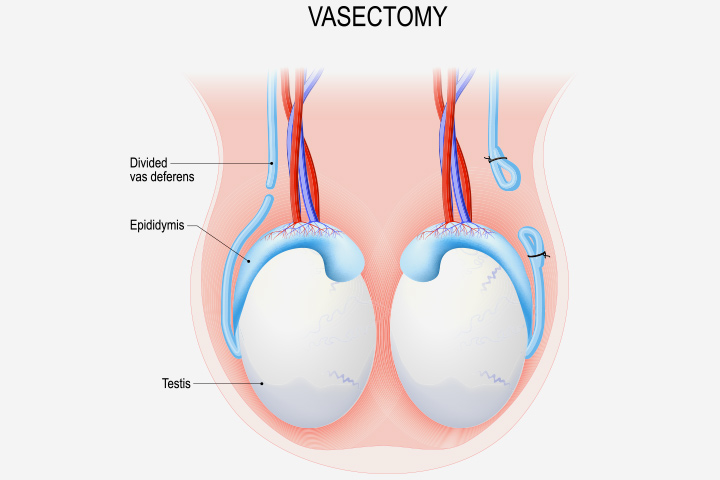
photo istock
Two conditions have to be met for a successful vasovasostomy.
1) The patient must have sperm available to pass through at least one reconnection and
2) Each connection must be watertight as possible to prevent scar tissue from forming.
VASOEPIDIDYMOSTOMY-
This procedure can also be called Epididymovasostomy. This is done only when a test has been carried out on the vassal fluid, and the findings shows Epididymal obstruction, it is often done when vasovasostomy fails, and also when there is no sperm present in the Vas deference.
It involves the connection of the severed Vas deferens to the epididymis and it is more technically demanding than the vasovasostomy. It attaches the Vas deferens directly to the epididymis above the point of blockage, the epididymis is inspected and an individual tubule is selected to enter and connect to the Vas deferens, from this point anyone out of two techniques can be used.
There are two technique to this approach;
Mucosa- to-Mucosa end-side method- In this method, an opened epididymal tubule is connected to the severed end of the Vas deferens with four to six small simple sutures, placed around the girth of each tubule.
Invagination vasoepididymostomy- here one to three sutures are placed near the opening of the epididymal tubule to allow the epididymal tubule to invaginate into the Vas deferens. The invagination technique has been said to have a higher chance of success and an improved watertight seal, theoretically though.
The success of vasoepididymostomy is highly dependant on the proficiency of the surgeon. Swelling, pains, and bleeding are likely to occur after vasectomy reversal, it is important to report this discomfort immediately to your doctor.
After a vasectomy reversal, it is advised to wear a hockey strap for support for about four to six weeks, and also abstain from strenuous activities for a while.
There are risk factors that affect the success rate of vasectomy reversal, hence the possibility of pregnancy, some of these risk factors include:
✓ Age of the female partner and the couple’s fertility potential.
✓ The method of reversal used
✓ The experience of the surgeon carrying out the procedure.
✓ The length of the Vas deferens left on the testicular end.
✓ The presence of inflammatory response after vasectomy= The presence of a sperm granuloma, a lump created by extravasated sperm after vasectomy has been found to be an indicator of vasectomy success.
✓ The length of time that has elapsed since the vasectomy was performed.
✓ Occlusion of the Vas deferens two or more years after the operation.
The success rate of vasectomy reversal is 90% according to a report in the Asian Journal of andrology.
Also after vasectomy reversal, an average of 90% will regain sperm after three to six months and an average of 73% will achieve pregnancy after a year according to Herrel LA, Good man M, Goldstein M, Haio W. outcomes of microsurgical vasovasostomy for vasectomy reversal: a meta-analysis and systematic review.
After the vasectomy reversal procedures, sperm evaluation is done later on. Once sperm counts return to adequate levels, the chance of pregnancy increases.
The second approach to achieving pregnancy after vasectomy is
SPERM RETRIEVAL
This is a way by which sperm is extracted from a male individual for either storage or to be used freshly, for either artificial insemination or in-vitro fertilization, for the purpose of achieving pregnancy.
There are different methods of sperm retrieval or harvest, a method is chosen based on where the sperm is to be extracted, what the individual wants, the capabilities of the surgeon in charge.
Before and after vasectomy the individual can retrieve his sperm and store using a process called cryopreservation, this special process would be explained later on in this article so stay tuned.
SPERM RETRIEVAL METHODS
1) NON-SURGICAL SPERM RETRIEVAL
If the collection of sperm is to done before vasectomy, no severance of male parts have been made, sperm can be collected naturally, by masturbation, interrupted intercourse, and other ways to get the male ejaculate and produce semen containing sperm, no lubrication should be used!
This sperm is collected in a special sterile laboratory container or a special type of collection condoms, that do not contain spermicide. The sperm should be taken to the laboratory within one hour if the collection was not done within the laboratory.
Ejaculation can be induced too if the individual has retrograde ejaculation or Anejaculation. Ejaculation can be induced using
PENILE VIBRATORY STIMULATION- done with a special vibrator placed at the top of the penis, this stimulation can cause the ejaculation of sperm naturally.
ELECTROEJACULATION- This is done with a prob that sends electrical energy to the prostrate and seminal vesicles inducing ejaculation.
Testicular sperm aspiration (TESA)-
A thin needle is used to puncture the tested to gently pull out sperm, no other cut is needed, a nerve block( an anesthetic into the nerves to treat pain) is used.
Micro Epididymal Sperm Aspiration– sperm is removed from the Epididymal tubes, using a needle
Percutaneous Epididymal sperm aspiration- here the urologist sticks a needle attached to a syringe into the epididymis to gently remove sperm, however, sperm may not always come out this way.
MICROSURGICAL SPERM RETRIEVAL
Testicular sperm Extraction- this is done in an operating room, this way more of the testis is examined, less tissue is removed, also less damage is done to the blood vessels, making several cuts and incisions in the testis and examining the tubules for the presence of sperm.
Microdissection testicular sperm extraction- this is also the extraction of sperm from the seminiferous tubules of a male testis. Most times 60% of sperm is found using this method.
Risk factors of sperm retrieval include
*Testicular injury or loss
*The chance of not finding sperm
* Infection and pains
* The need for future procedures.
The sperm collected can be used fresh or cryopreserved.
Cryopreservation-
This is the process of cooling, preserving, and storing cells, tissues, & organelles. in this case, sperm cell at a very low temperature to maintain their viability. The sperm stored can be used successfully indefinitely afterward. Frozen sperm lives only up to 24 hours inside the uterus as opposed to fresh sperm that can stay several days.
After the retrieval of sperm, it can then be used for either ARTIFICIAL INSEMINATION OR IN-VITRO FERTILIZATION.
Artificial insemination-
This is a fertility treatment method by which sperm is delivered directly to the cervix or uterine cavity for the purpose of achieving pregnancy. There are two approaches to artificial insemination;
- Intrauterine insemination (IUI)- this approach involves inserting retrieved sperm directly into the uterus, near the time of ovulation. prepared or washed sperm is used, a special catheter is used to insert the sperm.
- Intracervical insemination (ICI)- sperm is inserted into the cervix, care is taken to ensure that the tip of the syringe is as close to the entrance of the cervix as possible, also a cervical cap can be used for the insertion of sperm.
These procedures should be done by a doctor.
According to an article in a journal of andrology, pregnancy success rates for IUI are higher after 6 cycles of IUI compared with the same number of ICI cycles.
IN-VITRO FERTILIZATION (IVF)- this involves the extraction of eggs from a woman’s ovaries and sperm from a man. The sperm is used to fertilize the eggs in a lab, under controlled conditions, when the eggs grow as embryos, the embryos are then transferred to the woman’s uterus. This method is more invasive than artificial insemination.
IVF involves 2 ways of fertilization
- The traditional insemination- healthy sperm and mature eggs are placed in a petri dish,
incubated overnight and the sperm penetrate the eggs naturally in a culture media.
- Intracytoplasmic sperm injection(ICSI)- A single healthy sperm is injected directly into
mature eggs, using a micropipette. This method can be used if eggs have not been
fertilized by the traditional method.
Both IVF and artificial insemination do not guarantee a pregnancy. Using retrieved sperm for any of these procedures makes timing very crucial.
Risk factors of IVF
* Premature delivery and low birth weight
* Egg retrieval procedure complications.
* Multiple births.
In all these procedures listed above the possibility of pregnancy depends on;
✓ Age
✓ Overall reproductive health of the couple.
✓ The total motile sperm count.
✓ The success of the procedure.
Therefore with any of the above-listed approaches, it is possible to achieve pregnancy after vasectomy.
This article is not a guideline for any of the procedures highlighted! you have to speak with your doctor extensively to determine your best option.
ALSO, READ 14 Possible Benefits Of Drinking Coconut Water In Pregnancy
REFERENCE
- MEDICAL NEWS TODAY-https://www.medicalnewstoday.com/articles/326737
- WEBMD-https://www.webmd.com/sex/birth-control/news/20040505/vasectomies-pregnancy-prevention
- VERY WELL FAMILY-https://www.verywellfamily.com/getting-pregnant-after-vasectomy-reversal-4153916
- UROLOGY HEALTH- https://www.urologyhealth.org/urology-a-z/v/vasectomy
Originally posted 2020-11-06 13:22:23.

-

 Text Messages2 years ago
Text Messages2 years agoBEST LOVE CONFESSION MESSAGES FOR HER OR HIM
-

 Health2 months ago
Health2 months ago5 Unknown Ways To Maintain Skin Health
-

 Sex Education3 days ago
Sex Education3 days ago10 Simple Hack to Make a Girl Send Her Nudes
-

 Text Messages2 years ago
Text Messages2 years agoHappy Birthday Cousin, wishes and messages
-

 Text Messages2 years ago
Text Messages2 years agoHeart Touching RIP Uncle Quotes
-

 Uncategorized1 month ago
Uncategorized1 month agoHOW TO KISS A BOY FOR THE FIRST TIME
-

 Text Messages2 years ago
Text Messages2 years agoFreaky and Dirty Paragraphs For Him Copy And Paste Yahoo
-

 Text Messages2 years ago
Text Messages2 years agoBest Good Luck Wishes Before and After Surgery, for Family and Friends













